Nearly a year into the COVID-19 pandemic, and while far too many people have lost their lives or are suffering long-term symptoms, today’s light-based technologies offer hope by advancing methods of disinfection, diagnostics, treatment and more.
Disinfection
University of New Mexico researchers found that combining certain polymers and oligomers with UV light creates a coating that is effective at killing coronavirus on surfaces. when combined with UV light, to almost kill the coronavirus completely. The way it works is that the light activates the “docking” process that is necessary for placing the oligomer or polymer at the surface of the virus particle, allowing the absorption of light that generates the reactive oxygen intermediate at the surface of the virus particle.

A bonus is that the coating does not wash away with water and leaves no toxic residue. This technique can be applied in many ways including in personal protective equipment, sanitizing wipes, etc.
Read more about the research in “Researchers Combine Light with Polymers and Oligomers to ill SARS-CoV2”.
In another study, Sensor Electronic Technology, Inc. and Seoul Viosys recently demonstrated that UV LED technology could be an effective method to disinfect airborne viruses, water systems, as well as areas where COVID-19 patients were housed, including hospital rooms. The Violeds technology was shown to n quickly and effectively kill 99.437% of SARS-CoV-2 in less than one second, and the research team observed the inactivation rate of virus particles at 99.437% in one second.
Violeds, an advanced compound semiconductor technology, is an economically advanced and safer solution for the replacement of
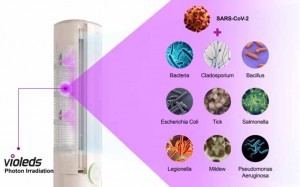 conventional UV lamps that contain mercury, a toxic element which does not dissolve and accumulates in the human body, is released when UV lamps are broken. Because of their short lifespan of around 5,000 hours, conventional UV lamps require frequent replacement. However, UV LED technology has advantages in both cost and safety with a long life of up to 50,000 hours, which is more than 10 times the life of conventional mercury lamps.
conventional UV lamps that contain mercury, a toxic element which does not dissolve and accumulates in the human body, is released when UV lamps are broken. Because of their short lifespan of around 5,000 hours, conventional UV lamps require frequent replacement. However, UV LED technology has advantages in both cost and safety with a long life of up to 50,000 hours, which is more than 10 times the life of conventional mercury lamps.
Read more about Violeds technology in “UV-LED Technology Can Kill 99% of Coronavirus in Less than a Second”.
Diagnostics
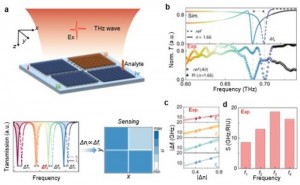
The coronavirus vaccines bring hope that our isolation will subside, travel will resume, and we will spend much needed time with family and loved ones. As we move toward broader immunity, antibody testing will become increasingly important. A team at the University of Rochester (New York) are working on a new approach to antibody testing, which so far has shown much promise.
Key to the technology is an optical chip, no larger than a grain of rice. Proteins associated with eight different viruses, including SARS-CoV-2, are
 contained in separate sensor areas of the chip. If someone has been exposed to any of the viruses, antibodies to those viruses in the blood sample will be drawn to the proteins and detected.
contained in separate sensor areas of the chip. If someone has been exposed to any of the viruses, antibodies to those viruses in the blood sample will be drawn to the proteins and detected.
“This is a completely new diagnostic platform,” says Miller, the Dean’s Professor of Dermatology and a professor of biomedical engineering, optics, and biochemistry and biophysics. “We think this is going to be valuable in very broad applications for clinical diagnostics, not just COVID-19.”
The card will enable clinicians not only to detect and study COVID-19, but also to better understand potential relationships between COVID-19 infection and previous infections and immunity to other respiratory viruses, including circulating coronaviruses that cause the common cold. The researchers will use blood drawn from 100 consenting convalescent COVID-19 patients to test the device’s effectiveness. When the researchers complete and validate the initial prototype, they will be able to apply for up to $5.3 million in additional funding to move the technology closer to commercial availability.
Read more about this research in “Chip on a Card Would Detect COVID-19 Antibodies in a Minute”.
Treatment
Based on the theory that laser light is able to relieve inflammation and promote healing in lung tissue, Photobiomodulation Therapy (PBMT) n PBMT, light is applied over damaged tissues, and light energy is absorbed by cells starting a cascade of molecular reactions that improve cell function and enhance the body's healing process.
PBMT has demonstrated anti-inflammatory effects and is emerging as an alternative modality in pain management, lymphedema treatment, wound healing and musculoskeletal injuries. The use of supportive PBMT for COVID-19 is based on the theory that the laser light reaches the lung tissue to relieve inflammation and promote healing. Additionally, PBMT is non-invasive, cost-effective, and has no known adverse effects.
The research was led by Scott A. Sigman, M.D. an orthopedic specialist based in North Chelmsford, Massachusetts (US). How does an orthopedist get involved with a COVID-19 study? He is familiar with the MLS laser’s ability to reduce inflammation from an injury, and because COVID-19 causes acute inflammation, he thought of testing MLS laser on COVID-19 patients. After receiving a non-significant risk declaration from the FDA, he teamed with a world-renowned cellular biologist, Professor Monica Monici as well as a world authority on photobiomodulation, Dr. Soheila Mokmeti from Canada. Dr. Mariana Vetrici was also on the team that created a randomized control pilot trial using MLS laser as supportive therapy for COVID-19 patients at Lowell General Hospital in Lowell, Massachusetts.
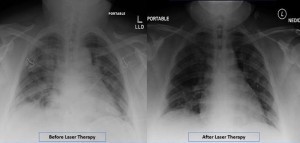
The patient, a 32-year-old Asian woman diagnosed with SARS-CoV-2, was treated with once-daily, 28-minute PBMT sessions for four days using an FDA-cleared Multiwave Locked System (MLS) Therapy Laser (ASA Laser, Italy). Prior to treatment, the patient had shortness of breath and difficulty with activities of daily living. Upon completion of treatment, the patient was able to independently ambulate and greatly improved her ability to perform activities of daily living. Two days following the final treatment, the patient was discharged with minimum supportive oxygen. Two days after being discharged, the patient was weaned to room air.
Read more about this study in “Doctors Using Laser Therapy to Treat COVID-19 Patients Report Positive Outcomes”.
Security
In a world in which we are increasingly dependent on the ability to identify those involved with criminal acts, the widespread use of face masks might impede proper identification. However, a new study of face recognition technology created after the onset of the COVID-19 pandemic shows that some software developers have made demonstrable progress at recognizing masked faces.

The findings, produced by the National Institute of Standards and Technology (NIST), are detailed in a new report. It is the agency’s first study that measures the performance of face recognition algorithms developed following the arrival of the pandemic. A previous report from July explored the effect of masked faces on algorithms submitted before March 2020, indicating that software available before the pandemic often had more trouble with masked faces.
“Some newer algorithms from developers performed significantly better than their predecessors. In some cases, error rates decreased by as much as a factor of 10 between their pre- and post-COVID algorithms,” said NIST’s Mei Ngan, one of the study’s authors. “In the best cases, software algorithms are making errors between 2.4 and 5% of the time on masked faces, comparable to where the technology was in 2017 on non-masked photos.”
Findings include lower error rates were generated by masks that cover only the mouth and nose, with higher error rates from wide mass that stretch across the cheeks; mask colors affect the error rate; and error rates are lower if an original saved image showed a masked face. It was also found that a few algorithms perform well with any combination f masked or unmasked faces.
Read more about this study in “Facial Recognition Accuracy with Face Masks.”
Written by Anne Fischer, Editorial Director, Novus Light Technologies Today

















 Back to Features
Back to Features