
Members of a UK-based EPSRC (Engineering and Physical Sciences Research Council) interdisciplinary research team called Proteus have developed a new type of system that can detect light from a source deep inside the human body.
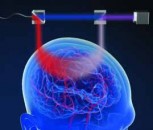
Led by Professor Robert Thomson and Postdoctoral Researcher Dr. Mike Tanner from Heriot Watt University in Scotland, the camera has been designed to highlight how doctors might be able to track a medical tool such as the illuminated tip of an endoscope. Until now, it has not been possible to track where an endoscope is located in the body in order to guide it to the right place without using X-rays or other expensive methods.
Capturing visible light emanating from inside the body, however, is not a trivial task. Fortunately, in the near infrared range between 700 to 900 nm, the absorption coefficient of tissue is reasonably low, at less than 0.1 cm-1.
“Although light within this range can be detected through several centimeters of tissue, the majority of the light is scattered as light bounces off the tissues in its path, diffusing the light and reducing the spatial information that can be transmitted from an embedded source to an external detector. This makes conventional through-tissue imaging practically impossible, as the scattering results in a blurred image and loss of information,” said Dr. Tanner.
Custom-built camera
To resolve the scattering issue, the Proteus researchers developed a custom built camera that can be deployed to detect just a small fraction of photons that escape the tissue with low scattering. These so-called “ballistic and snake” photons scatter relatively little and travel in a nearly direct (or ballistic) path to the camera, arriving much sooner than their scattered counterparts.
The camera itself employs an array of Single-Photon Avalanche Diodes (SPADs) built on a CMOS substrate that was designed at the Department of Electrical Engineering at the University of Edinburgh and manufactured by ST Microelectronics.

A UK-based interdisciplinary research team called Proteus hope that the camera they are developing could eventually be used to help physicians locate light sources from the tips of endoscopes that have been inserted into the human body.
Megaframe SPAD detector
To reduce ambient light from its surroundings, the so-called “Megaframe” SPAD detector was placed inside a metal box and a filter was placed in front of an aspheric lens used to focus light onto the imager to reduce the influence of room lighting.
To demonstrate the effectiveness of the system, a 785 nm Picoquant fibre coupled laser diode passed light into an optic fibre probe (an analogue of a medical device) placed inside a variety of tissue types to create a pulsed light source with a repetition rate between 20 MHz and 80MHz. Having travelled through the tissue, the photons of light impinge on the SPAD pixels on the imager in the camera, triggering an avalanche current.
“The leading edge of the avalanche pulse marks the arrival time of the detected photon, which is detected with 50 picosecond resolution by dedicated timers associated with each of the pixels on the SPAD. A timer is started by the detection of a single photon, and stopped by the arrival of a trigger derived from the timing of the laser pulses. From the two timings, the precise time of flight of a single photon can be determined,” said Dr. Tanner.
Using Time Correlated Single Photon Counting
While conceptually straightforward, in reality the actual number of photons from each pulse of the light source that reach the detector in the camera are orders of magnitude too small to enable any useful measurement to be made. As a result, a well-established technique called Time Correlated Single Photon Counting (TCSPC) was employed to address the issue. With this technique, the intensity of the output signal from the system is derived by counting the number of output pulses within a measurement time slot over many repeated laser pulses.
As the photons generated by the laser reach each of the pixels in the camera, their arrival time is measured. The timing data is then collated into a set of a time bins, each with 50 picosecond widths. The photons that arrive at a pixel detector the fastest are the ones that have taken the most direct path to the pixel in the imager from the light source, having been scattered the least by the tissue. Those photons that arrive at the detector at later times, on the other hand, will be those that have been scattered more by the tissue they have travelled through.
“By making numerous measurements of photon time arrivals over a specific time period, enough photons will be counted by the SPAD detector to provide meaningful information. By creating a histogram showing the number of photons that arrive in each of the time bins, it is then possible to derive an image snapshot from the early ballistic photon arrival times to determine the location of the light source to within cm resolution,” added Dr. Tanner.
The rate at which the laser was pulsed was chosen so that the arrival of individual photons could be measured by the system before any photons following from the subsequent laser pulse arrived. In doing so, the researchers could be sure that the histograms that were constructed would accurately represent the photon arrival times transiting the system within a given time window.
Measurement accuracy
According to Dr. Tanner, at the present time, the system is unable to provide the same level of millimeter accuracy that can be obtained by contemporary electromagnetic systems that detect wired coils integrated into medical devices. When fitted with a Thorlabs aspheric lens with a focal length of 4.6mm to image a 30cm field of view onto the 1.6mm square detector array, the Heriot-Watt system was able to deliver measurement accuracy to within centimeter accuracy.
“One reason for this is that the SPAD imager in the present system only sports 32 x 32 pixels, whereas most contemporary CMOS imagers have many megapixels. As a result, we believe that the resolution of the system is limited by the relatively low number of pixels. However, in the next prototype of the system, we plan to employ a SPAD device with more pixels to improve the resolution,” said Dr. Tanner.
Another important factor that may limit the resolution of the system is how accurately it can time the arrival of photons. Clearly, the more accurately the arrival time can be measured, the easier it becomes to discriminate between those photons that are ballistic and those that have been scattered by the tissue. Dr. Tanner said that the research team plan to investigate how arrival times affect image resolution as they develop a next-generation camera based on a higher resolution SPAD imager.
To determine the potential interference from significant muscle and bone structure, the researchers used their camera to capture images of light traveling though a number of different types of models of a chest and lung as well as demonstrating the technique through the entire thickness of a human torso. The prototype demonstrations showed that a point light source can be located through tissue approximately 20 cm thick under normal lighting conditions using the ballistic imaging technique.
The new system is reasonably compact, comprising a tripod mounted camera and a laser pulsed source, and can even be used within an environment with fluorescent room lights. The researchers believe that the simplicity of the approach will eventually enable ballistic photon localization to move out of the lab and into the clinic. The camera will be developed further to enable clinicians to locate inserted medical devices at the bedside, visualizing both the tip and length of the device.
Written by Dave Wilson, Senior Editor, Novus Light Technologies Today



















 Back to Features
Back to Features



























